 While Topol is overall very enthusiastic about this research, he does have some concerns. "I think it may wind up giving us a whole new map for what to do in terms of drugs and vaccines, which is really notable." Eric Topol, a physician-scientist at the Scripps Research Institute who wasn't involved in the study. The scientific community is raving about the new study. The study doesn't have all the answers but could hold clues to better COVID treatments If you show the immune system a piece of a virus, it can use that as a template to create "Memory T cells." which can recognize viruses in future infections that match the template and start an immune response. :no_upscale()/cdn.vox-cdn.com/uploads/chorus_image/image/66594939/Symptoms.0.jpg)
This is similar to how many vaccines, including the COVID vaccine, work. "The thinking is that your exposure to some seasonal cold viruses, that in some cases share a lot of similarities with parts of SARS-CoV-2, gave you some existing immunity," Hollenbach says. That's the result of a process called cross-reactive immunity. The research shows that people with HLA-B*15:01 have an enhanced protection against COVID after being exposed to closely related common cold viruses. "But it was a really clear, robust and replicable association." They call it 'cross-reactive immunity' "To be fair, not everybody that has will be asymptomatic," Hollenbach says. Hollenbach found that one of them, HLA-B*15:01, was associated with asymptomatic COVID. There are hundreds of different HLA variants. When we're infected by a virus, HLAs will hold out a piece of that virus like a flag, telling the immune system to kill the infected cell. HLAs are a class of genes involved in the immune system that sit on the surface of our cells. "There's more diseases and conditions associated with variation in the HLA genomic region than any other genomic region. Hollenbach thought that the same HLA genes used to find bone marrow matches could also be involved with COVID outcomes. "We simply asked people who were registered donors to track their COVID experience through a smartphone app and consented to let us look at their genetic data and link it to their answers," Hollenbach says. Some people who had provided a DNA sample to the program also signed up to participate in Hollenbach's COVID-19 Citizen Science Study. 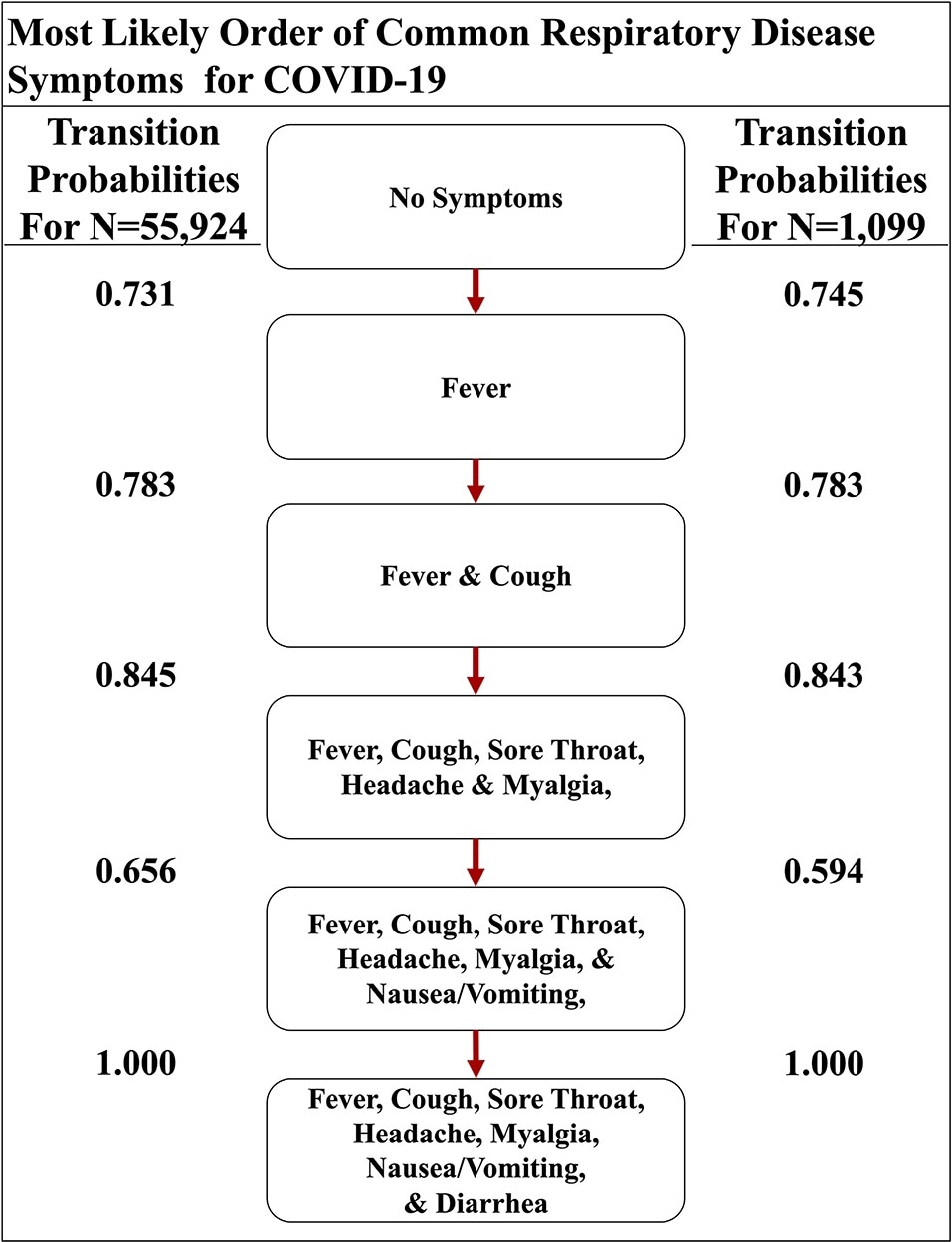
The new findings are thanks, in part, to the Good Samaritans who signed up to donate bone marrow through the Be The Match program. We really haven't understood what's driving that," she says. And the other end of that spectrum is you didn't have any symptoms. But in her research, she says she's most interested in those with extreme cases. 
Hollenbach had a common kind of COVID experience, moderate symptoms and eventually a full recovery. Jill Hollenbach, an immunologist at the University of California, San Francisco who led the research described in the new study, didn't have a mild COVID experience. many common colds, and thus know how to attack COVID-19 too. Since then, the scientists have found out how this genetically enhanced protection works – it's because of immune cells that remember infections from other seasonal coronaviruses, i.e. Goats and Soda covered an early version of this study last year. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
